Advancing Diagnostics for Patients with Neurological Disorders
Future Products & Concepts
Neurolign’s next-generation systems are designed to seamlessly capture and share high-fidelity eye movement data with medical professionals for interpretation.
DX 200
Neurolign is continually improving DX 200 hardware and plans to introduce a second-generation system. The DX 200 is a head mounted goggle (HMI) with high-speed eye tracking system using a dual camera approach and a high-resolution display. DX 200 will provide visual and auditory stimuli to patients through HMI and tracks. The device will seamlessly record and share eye movement data with medical professionals for interpretation.
Proposed System Features
QCS 610 Based SoM, running Android IOT
Wireless Joystick (Option for wired)
Status Lights and Single Button on Outside
USB-C Port for DFU, and tethered usage
Single Display (HD)
Speakers for Auditory instructions
Photo diode to synchronize display to camera
Dual camera simultaneous capture at 250FPS (one per eye)
Mechanics to Align Camera with eyes (no hot mirrors)

Featured Research
Neurolign utilizes industry-leading eye-tracking technology and expertise in neuroscience to develop innovative products that aid in the diagnosis and monitoring of neurological injury and disease.
Neurolign has developed a comprehensive battery of oculomotor, vestibular, reaction time, and cognitive (OVRT-C) tests delivered via the Neurolign DX 200, our high-resolution eye-tracking goggle set. Together, results of these tests can reveal the unique and quantifiable patterns of OVRT-C deficits characteristic of specific neurological injuries or diseases.
Our multimodal method of OVRT-C testing makes us uniquely positioned to develop adjunctive tools with which to diagnose and monitor a number of these conditions and potentially contribute to patient recovery. Below, we share results from recent studies that highlight the efficacy of our novel approach to help clinicians diagnose and treat patients.
Neurolign DX 200
Long COVID
Over two years into the COVID-19 pandemic, it is clear that neurological symptoms (e.g., “brain fog”, dizziness, smell and/or taste abnormalities) feature prominently on the list of patient complaints, both during COVID-19 infection and often following recovery. Neurolign tested 77 recovered COVID-19 patients with our comprehensive battery of OVRT-C tests to determine if neurological deficits related to COVID-19 infection can be objectively measured. A significant number of patients scored outside established norms on several of our tests. Based on the characteristic pattern of deficits observed in these subjects, we developed a model using six metrics that are significant indicators of post-COVID-19 patients. Recovered COVID-19 patients exhibit systematic deficits in smooth pursuit, optokinetic nystagmus, predictive saccade, and antisaccade metrics. Based on this pattern of deficiencies, we built a classification algorithm that can discriminate recovered COVID-19 patients from healthy controls at a high degree of accuracy. This technology may prove invaluable to the diagnosis and treatment of COVID-19-related neurological deficits following recovery from the acute phase of infection.
A manuscript reporting these data and results was recently published in Frontiers in Neurology.
Vestibular Migraine
Vestibular migraine (VM) is condition in which vertigo, dizziness, and/or balance issues occur in patients with a history of migraine. VM is particularly difficult to diagnose, as it relies heavily on subjective patient reports, its symptoms overlap with several other vestibular disorders, and there is currently no objective test for the disease. Using our battery of OVRT-C tests in patients with VM, we found robust deficits in these patients at the group level, such as abnormalities in saccades, smooth pursuit, vergence, and optokinetic nystagmus (see Figures 1-2 for examples of abnormal latency and velocity of saccades in VM patients; see Figure 3 for an example of abnormal vergence). A regression model generated from these data can discriminate between VM patients and healthy, age-matched controls with a high degree of accuracy. This algorithm may aid in the early detection of VM, which will help clinicians treat the condition earlier and improve patient outcomes.

Figure 1. Increased latency of horizontal saccades in a VM patient (normal mean latency <0.22 seconds)

Figure 2. Decreased velocity of horizontal saccades in a patient with VM (normal area under fit >8239)
Figure 3. Abnormal convergence and divergence in a VM patient. Symmetry values of +0.86 for convergence and +0.74 for divergence. A symmetry value of -1 indicates eyes are moving in perfectly opposite directions (normal), and a value of +1 indicates eyes are moving in perfectly parallel directions.
Diagnostics in Development
Neurolign is developing algorithms to identify patients with a variety of disorders with significant unmet diagnostic needs.
Concussion / mTBI
Concussion (i.e., mild traumatic brain injury/mTBI) is highly prevalent across a wide range of occupational, recreational, and athletic contexts and is a leading cause of neurological injury in the United States. When left undetected and/or improperly managed, mTBI can lead to long-term pathophysiological changes that can affect an individual’s ability to function physically, cognitively, and psychologically. Nevertheless, current diagnostic tools rely heavily on subjective reports and neuropsychological/neurocognitive testing (e.g., MRI), which can yield imprecise and/or inconclusive results and are time consuming, expensive, and not readily available in all environments (e.g., field side at athletic events). There is an unmet need for a fast, accurate, non-invasive, and portable tool to aid in timely diagnosis of concussion.
mTBI affects brain pathways that control or influence OVRT-C processes. Oculomotor and vestibular dysfunctions affect up to 90% of patients with acute TBI and have been shown to be predictors of outcomes for recovery as well as valuable measures of the severity of the injury. Symptoms associated with mTBI include a few disturbances to basic vision, reactions times, and cognitive processes.
Neurolign tested the OVRT-C performance of 106 patients diagnosed with mTBI and those of 300 healthy, age-matched controls aged 18-45 years. From these data, we were able to develop a Concussion Assessment algorithm based on six OVRT-C metrics from our test battery. The Concussion Assessment can be used as a reliable adjunctive tool to aid in the diagnosis and monitoring of mTBI. Importantly, the Concussion Assessment can be used with our Neurolign DX 200 goggles to alert individuals to the possibility of concussion regardless of their location, which will help improve the safety and care of athletes, workers, and children at play.
Neurolign is in the planning stages of a large-scale clinical trial with the goal of testing and strengthening our Concussion Assessment model.
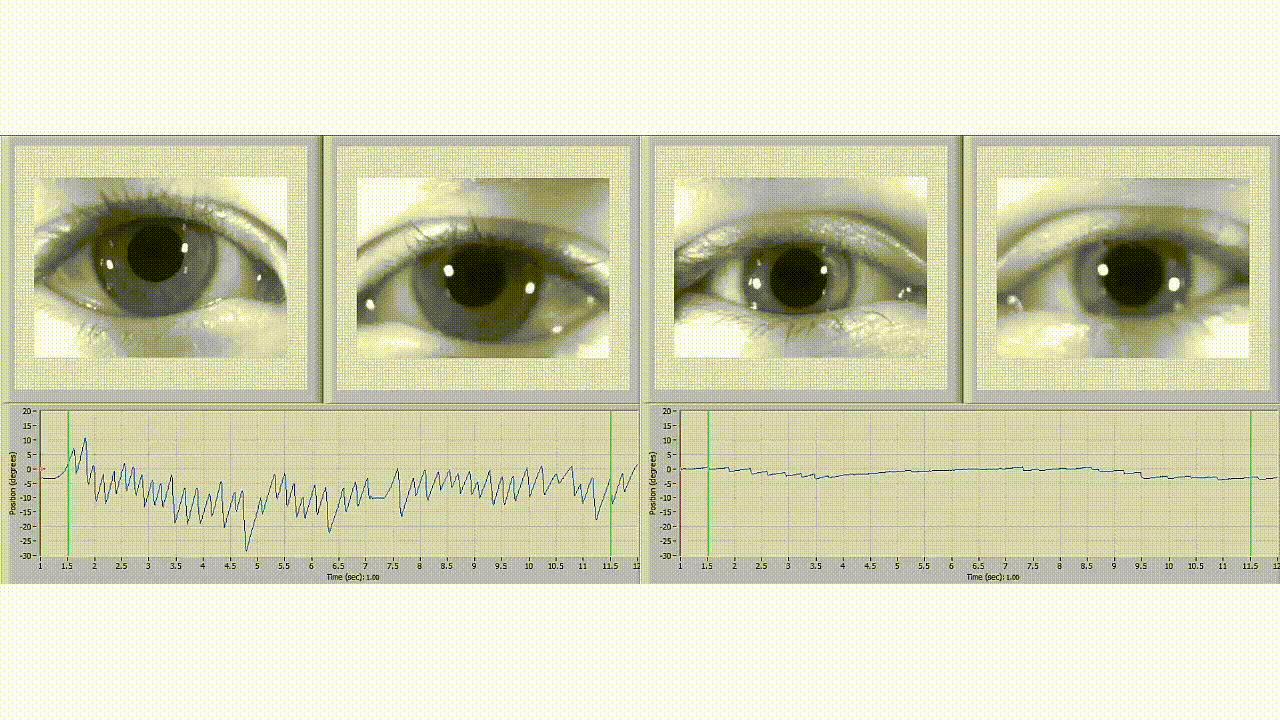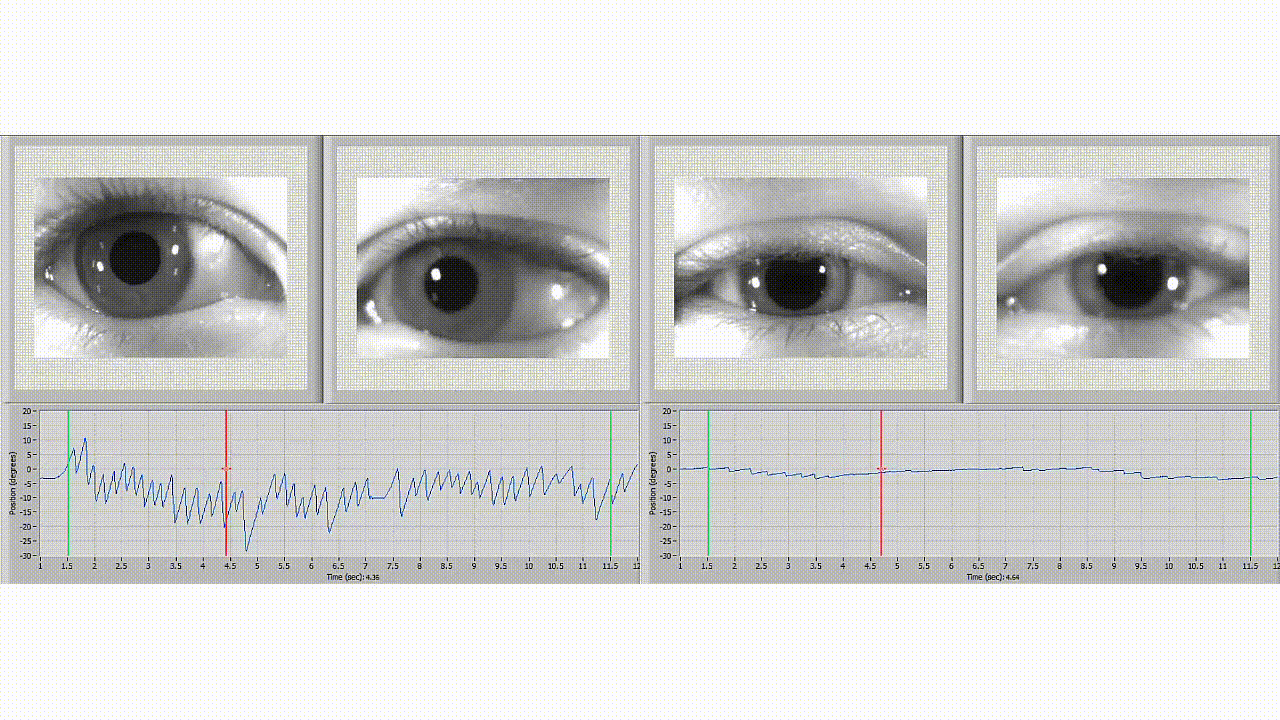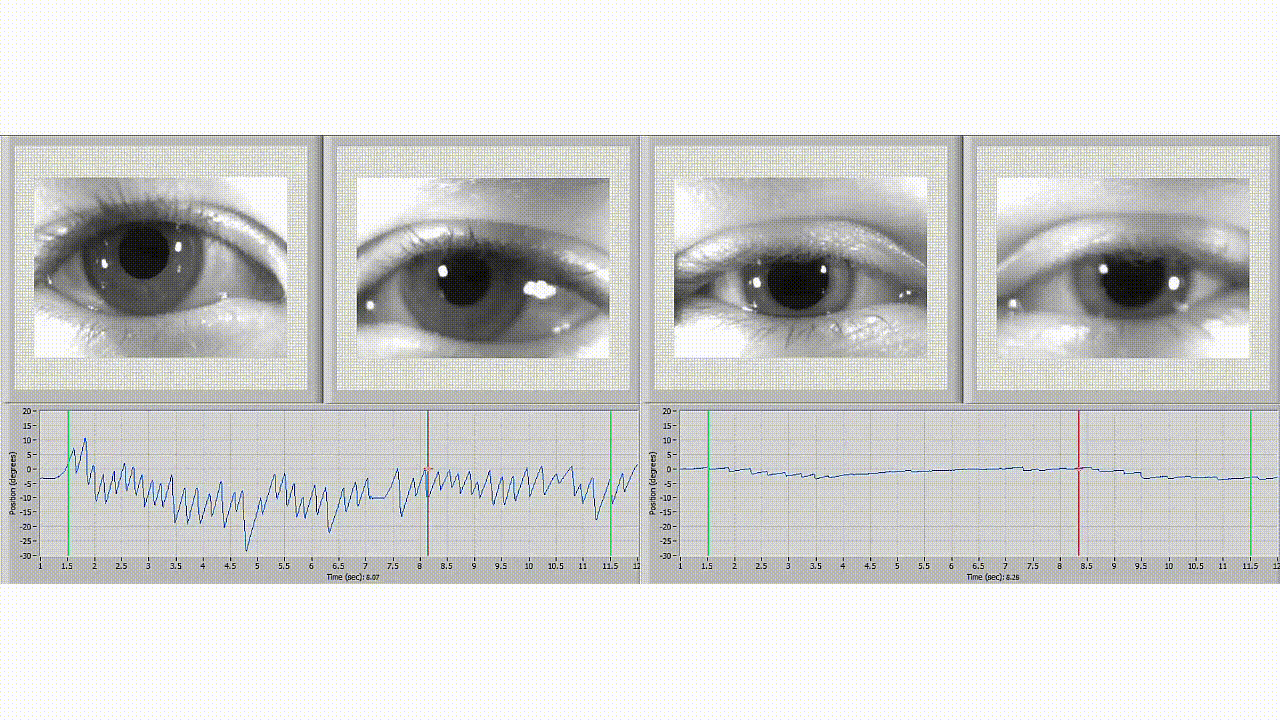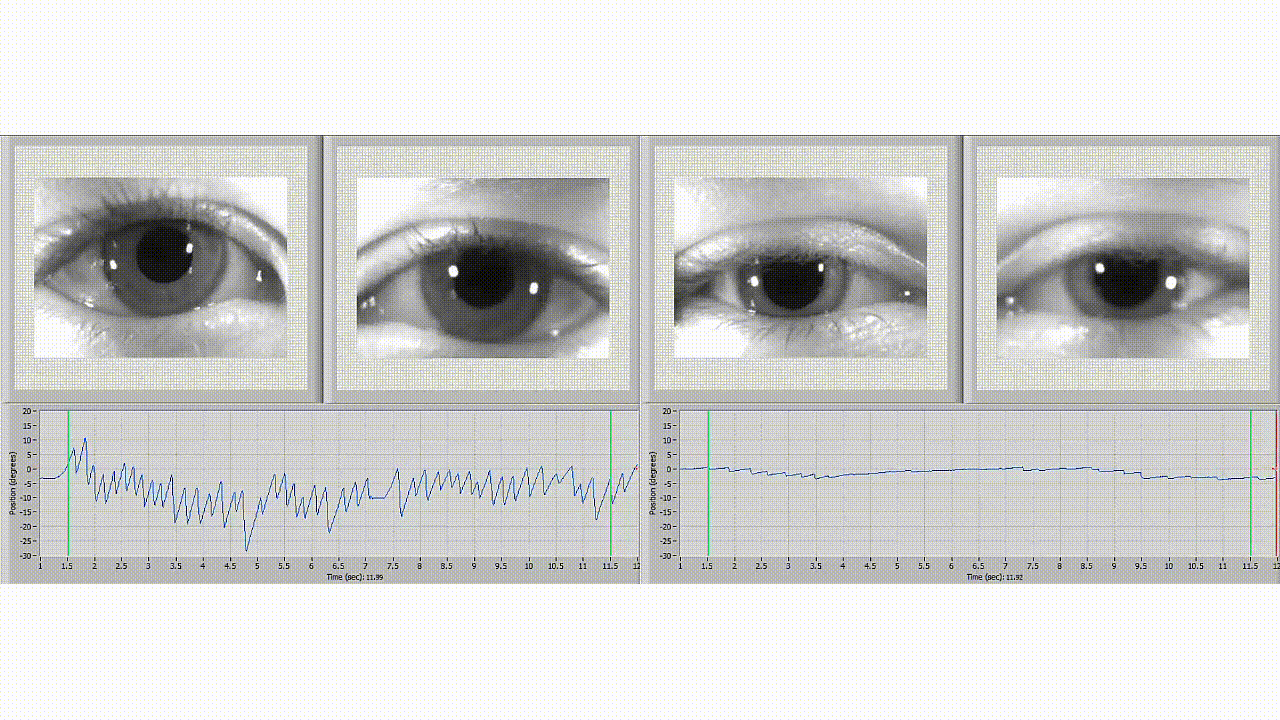
Neurolign software is used to differentiate between normal eye movement (left) and an individual with symptoms of concussion (right).
Multiple Sclerosis
Multiple sclerosis (MS) is a chronic autoimmune disease characterized by central nervous system (CNS) inflammation, demyelination, and axonal injury and loss. Current diagnosis of MS relies primarily on imaging techniques such as magnetic resonance imaging (MRI) and invasive techniques such as spinal fluid analysis and blood tests. Imaging techniques are time-consuming and expensive and provide only structural information that may not correlate with function. Objective measures to diagnose and monitor disease progression are necessary. A pilot study conducted by Neurolign evaluated the use of OVRT-C tests as an adjunctive diagnostic tool for MS. 12 patients with MS performed our battery of OVRT-C tests, and their metrics were compared to Neurolign’s FDA-approved normative OVRT-C data to assess whether specific patterns of deficits can accurately distinguish MS patients from healthy adults.
Despite a small sample size, our preliminary results suggest these patients exhibit noteworthy deficits in Saccades, Binocular Vergence, Smooth Pursuit, Pupillary Light Reflex, and Gaze Horizontal performance. We continue to test patients with our MS protocol and expect to use these data to develop an MS algorithm that can be utilized in clinical settings to identify MS patients easily and objectively.
Left: A screenshot of the prototype VEST™ software that assesses saccade disconjugacy in duration, amplitude, and velocity, which are particularly abnormal in MS patients. Right: For comparison, saccade disconjugacy results for a healthy control subject.
Mild Cognitive Impairment
Mild cognitive impairment (MCI) is characterized by cognitive deficits beyond those experienced in normal aging that are not yet severe enough to interfere with daily life (e.g., deficits in memory, thinking, language, and/or judgement) but are often a precursor to Alzheimer’s disease (AD). As there is currently no specific test to confirm suspected MCI, clinicians must rely on self-reported symptoms and a range of various tests for diagnosis. Patients with MCI exhibit well-documented OVRT-C deficits, such as atypical saccades, impaired antisaccade performance, increased visual and auditory reaction times, and abnormal pupil constriction and relaxation. Neurolign is currently testing MCI patients and healthy, age-matched controls using a battery of 19 OVRT-C tests to determine if statistical modelling can be used to identify characteristic patterns of OVRT-C deficits that are unique to MCI patients.
While this study is ongoing, preliminary results suggest that deficits in Antisaccade, Vergence, Self-Paced Saccades, Memory-Guided Saccades, and Visual Paired Comparison performance may be characteristic of patients with MCI. A statistical algorithm that can detect MCI using a simple, 15-minute OVRT-C battery of tests will be an invaluable adjunctive diagnostic tool for clinicians seeking to diagnose MCI at early stages and potentially mitigate or slow the progression from MCI to AD.
Parkinson’s Disease
Parkinson’s disease (PD) is a progressive neurodegenerative disorder that affects movement. Common symptoms include tremors, stiffness, and slowness of movement that begin gradually and worsen over time. Diagnosis of PD is made based on the medical history of the patient combined with neurological and physical examinations; however, diagnosis is subjective and challenging as PD symptoms vary considerably between patients and often overlap with other diseases. As a result, it is not uncommon for patients with PD to misdiagnosed at least once, which delays treatment and can negatively affect patient outcomes.
Given the effects of the disease on motor control, many oculomotor behaviors are impaired in patients with PD. Abnormalities in saccades, vergence, smooth pursuit, memory-guided saccades, optokinetic nystagmus, and antisaccades are well-documented, and notable cognitive deficits are common. While scientists are aware of these deficits, no singular OVRT-C biomarker for PD currently exists. This may be because independently, these features are not sensitive or specific enough to accurately indicate a PD diagnosis; however, the ability to identify a pattern of OVRT-C results that is unique to PD patients would have valuable utility as an objective biomarker for PD.
Tasks in Neurolign’s test battery are designed to assess OVRT-C functions known to be affected in individuals with PD. Neurolign is currently conducting a pilot study to evaluate the hypothesis that the disease is characterized by a quantifiable pattern of OVRT-C deficits. If our hypothesis is correct, collected data will be used to develop a classification algorithm able to identify patients with PD at a high level of accuracy. Such an algorithm will accelerate the diagnosis of PD and ultimately contribute to improved patient care and outcomes.
Strabismus
Strabismus is a visual disorder that affects control of eye movement and causes a misalignment between the two eyes. Ocular alignment problems are common in children and adults, and can often cause double vision, headaches, poor 3D vision, and low self-esteem. Measurements of eye movements and ocular misalignment in different gaze positions inform clinicians which extraocular muscles are functioning atypically and can illuminate the cause of muscle weakness or eye movement restriction and thus guide diagnosis and treatment. However, determining the cause and treatment plan relies on accurate determination of the pattern of misalignment in different gaze positions.
Neurolign is developing Dx100 software for automated, objective, reproducible motility, strabismus measurements, and afferent and efferent assessments of pupillary defects, which are also indicative of brain health. We will validate the automated measurements against current standard of care manual measurements of eye misalignments and pupil reactivity to light. We expect our results to support the introduction of field of binocular vision as an outcome measurement in the treatment of adult strabismus. Data from this study will allow us to create strabismus “maps” that show how disparities between the eyes change with gaze and allow clinicians to make more accurate diagnoses and design optimal treatment plans for strabismus patients.
A screenshot of the prototype VEST™ software that assesses horizontal and vertical misalignment in 9 cardinal gaze positions.
Featured Publications
Manuscripts
- Kelly K, Anghinah R, Kullmann A Oculomotor, vestibular, reaction time, and cognitive (OVRT-C) tests as objective measures of neural deficits in patients post COVID-19 infection. Frontiers in Neurology. 202210.3389/fneur.2022.919596.
- Kullmann A, Ashmore RC, Braverman A, et al. Portable eye-tracking as a reliable assessment of oculomotor, cognitive and reaction time function: normative data for 18-45 year old. PloS ONE. 2021;16(11):e0260351.
- Kullmann, A, Ashmore RC, Braverman A, et al. Normative data for ages 18-45 for ocular motor and vestibular testing using eye tracking. Laryngoscope Investigative Otolaryngology. 2021;6:1116-1127.
- Balaban CD, Szczupak M, Kiderman A, et al. Distinctive convergence eye movements in an acquired neurosensory dysfunction. Frontiers in Neurology. 2020;11:469.
- Kiderman A, Hoffer M, Szczupak M, et al. Oculomotor, vestibular, reaction time and cognitive eye-tracking mild traumatic brain injury assessment. Neurology. 2020;95(20 Supplement 1):S2.
- Balaban CD, Kiderman A, Szczupak M, et al. Patterns of pupillary activity during binocular disparity resolution. Frontiers in Neurology. 2018;9:990.
- Kelly KM, Kiderman K., Akhavan S., et al. Oculomotor, vestibular, and reaction time effects of sports-related concussion: video-oculography in assessing sports-related concussion. J Head Trauma Rehabil. 2018;34(3):176-188.
Events
American Academy of Neurology 2022 | Seattle, WA
- Oculomotor, vestibular, reaction time, and cognitive assessment in vestibular migraine
Neuroscience 2021 | Chicago, IL
American Balance Society 2020 | Scottsdale, AZ
- Oculomotor, vestibular, reaction time and cognitive (OVRT-C) tests in recovered COVID-19 patients
Patents
Title
Patent Number
A Quantum Shift in Brain Health and Wellness
Neurolign is on a mission to create a quantum shift in the clinical approach to neurodegenerative disease while simultaneously revolutionizing brain health and wellness.
